Gum Disease Treatment
Gum disease is a serious condition that affects people from all walks of life. Our dentistry provides periodontal services for all stages of gum disease to restore your oral health.
Periodontal Disease
Periodontal disease, periodontitis, and gum disease are all phrases used to describe an infection in the gums and bone surrounding your teeth. Healthy bone and gum structures help keep a tooth’s root intact. When food and plaque get trapped between the gums and teeth, it can lead to infection, resulting in gum disease. Periodontal disease is a very serious dental disease that affects many people. It is caused by bacteria from plaque formations on the teeth.
Gingivitis is an inflammation of the gums and one of the earliest stages of gum disease. Common symptoms of gingivitis include minor redness, swelling, or light bleeding of the gums. If left untreated, gingivitis turns into a more serious infection known as periodontal disease, which can lead to permanent structural damage.
Nearly half of all adults suffer from periodontitis to some extent—periodontitis is also referred to as gum disease and occurs when the gums are left exposed to harmful bacteria, tartar and plaque for an extended period of time. This can be caused by poor flossing habits and build-up between the teeth. If left untreated, it can progress and lead to bone and tooth loss.
-
What causes periodontal disease or gum disease?
Our mouths provide a home to millions of bacteria, both beneficial and harmful. Bacteria form a sticky substance, plaque, that adheres to the teeth. Brushing and flossing aim at removing plaque before it mineralizes into tartar. Tartar becomes a colony for more bacteria and adds to their population, pumping out toxins into the gums.
Gums react to this bacterial invasion with an inflammatory response under the direction of the immune system. Around the base of each tooth, a small collar of gum tissue exists that forms a small crevice or pocket. This warm, dark environment provides a perfect habitat for deeper tartar and bacterial penetration, with their toxins seeping into the base of the collar.
Early inflammation results in bleeding gums, known as gingivitis. Bacteria left untreated and undisturbed successfully create a chronic infection in the gum collar. In many cases, the bone begins to deteriorate around the teeth as the bacteria burrow deeper into the gums. While gums may be slightly tender at this stage, there’s generally minimal discomfort as the bone dissolves.
More than 50% of the bone around your teeth can disappear before any signs of looseness or pain begin to appear. The bone around teeth never regenerates, so this loss becomes permanent and harder to control as the bacteria hide deeper into the gums. Untreated gum disease leads to abscess and generalized tooth loss in many advanced cases.
-
How does a dentist identify if gum disease is present?
Identifying gum disease as early as possible is crucial to preventing bone and tooth loss. To determine if you have periodontitis, and its severity, we will:
- Review your medical history. Certain risk factors, such as genetics, taking certain medications or smoking, can increase the likelihood of gum disease.
- Exam your teeth and gums. If you have severe plaque/tartar build up or your gums bleed easily are both indicators that disease is present.
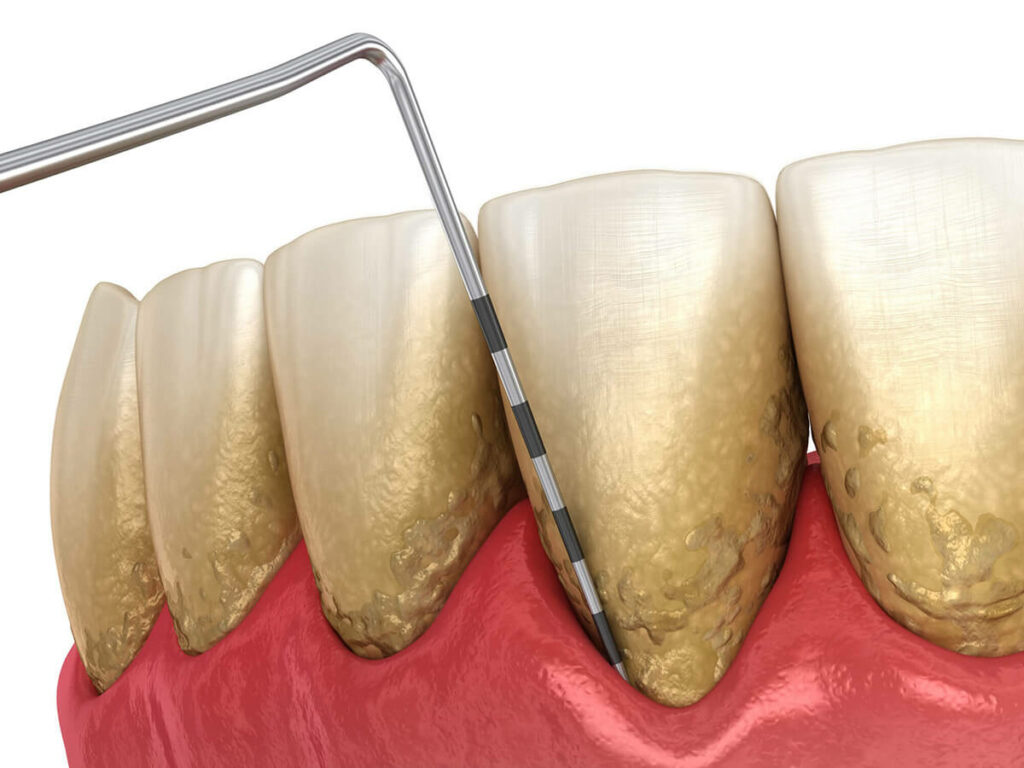
- Measure gum pocket depth. We place a dental probe between your teeth and gums, throughout different areas within your mouth.
- 1-3 mm is a healthy and normal gum pocket depth
- 3-5 mm is early or mild periodontitis
- 5-7 mm is moderate periodontitis
- 7-10 mm is advanced periodontitis
- Take x-rays of your mouth. Dental x-rays can reveal if you’ve suffered any bone loss in areas where deeper gum pocket depths are present.
-
How do I prevent periodontal disease or gum disease?
Regular home care is critical to arrest the progression of gum disease. Within a few hours of a careful cleaning, the bacteria begin to repopulate and adhere to the teeth. Plaque left undisturbed will start to harden and mineralize within 24 hours. And deeper gum pockets require even more diligence to prevent the bacteria from burrowing further into the foundation of your teeth.
Since the deepest sections of gum pockets previously damaged by bacteria can be difficult to reach at home, a particular maintenance schedule with us proves essential. We can customize your plan to include 2, 3 or 4 visits a year depending on the severity of disease and its response to treatment and home care.
If our combined efforts don’t halt your gum disease, we will suggest referral to a trusted specialist, known as a periodontist. With specialized training in many gum conditions, further treatment may be recommended.
Current research continues to establish clear links between bacterial disease in your mouth and ailments in other parts of the body. Studies show a link between oral bacteria and conditions such as heart disease, stroke, arthritis, Alzheimer’s, and certain types of cancers. The integration of oral and general health has never been better understood than it is currently.
Bleeding gums provide a direct pathway into the bloodstream, a journey that toxic oral bacteria can quickly take. In fact, if bleeding gums connected into one single patch, it would create a 2 x 2-inch square. If an open wound of this size existed on your skin, infection would be a concern. Bleeding, infected gums offer this open door to your body and sit saturated in colonies of bacteria. This helps explain why researchers continue to identify oral bacteria deposits in various areas of our bodies.
Diabetes and other auto-immune disorders lower the body’s ability to fight infection, allowing uncontrolled gum disease to advance faster and with more destruction. Research also confirms that the inflammation in the mouth can aggravate diabetes, making it harder to control. This two-way relationship between two chronic conditions emphasizes the importance of optimal oral health.
-
What is gum recession?
Receding gums affect about half of Americans over the age of 50. But, young people can experience gum recession too. You may be genetically predisposed to gum recession. Some people are born with thin gums. Other times the environment might contribute to recession. Things like aggressive brushing, trauma, surgery, or ill-fitting partials can cause recession.
Treatment of Gum Recession
If you notice a tooth looks long or you experience sensitivity or pain when brushing and flossing, you could have gum recession. Be sure to come in and have one of the doctor’s take a look. If you have recession we can typically graft a small amount of skin from your palate and patch it over the receding area. The treatment helps protect the tooth from further damage. It is a minor procedure that can be done for a single tooth or multiple teeth depending on your need.
What are you waiting for?
At Maynard Family Dentists, we believe in providing the best dental care, at the most affordable prices. Make an appointment, see more about our office, or explore all of the dental services we provide, using the links below.

